Hand hygiene, the most simple and effective infection control measure, is being neglected by doctors and nurses in more than 40% of situations where it is called for. This has been demonstrated by numerous studies across the world. In a recent study, where the staff did not know they were being observed, doctors and nurses only cleaned their hands 20% of the time when they should have.
Why is hand hygiene so important?
As health care workers we know that hand hygiene is standard practice in health care settings but do we really understand and acknowledge its significance?
The need for hand hygiene was first identified by Ignaz Semmelweis in 1847 when he drastically reduced puerperal sepsis by insisting that doctors and nurses in a maternity facility disinfect their hands. However, this was before Pasteur confirmed that organisms cause of infections.
Semmelweis, who is today recognized as the father of hand hygiene, was ridiculed by his fellow medical practitioners who eventually conspired to have him admitted to a mental institution.
Today there is abundant scientific evidence which shows that hand-hygiene alone can significantly reduce cross-infection in the healthcare environment.
The Centers for Disease Control in the United States (CDC) has estimated that every year 2.4 million Americans acquire infections in hospitals and that this leads to around 10,000 deaths. They believe that about half of these infections would be preventable by proper hand hygiene.
Health care acquired infections (HCAI) lead to increased hospital stays, huge financial burdens on the families and health services as well as unnecessary deaths. It also contributes significantly to increased numbers of antibiotic-resistant bacteria which are difficult if not impossible to treat.
The CDC has reported that most deaths from antibiotic resistance are from infections picked up in health care settings. The World Health Organization has declared antimicrobial resistance as a potentially catastrophic global public health threat and it is strongly advocating back-to-basics infection control measures – the most important being proper hand hygiene.
How does hand hygiene prevent infections?
Five conditions have to be present for pathogens to be transmitted within a healthcare setting. These are:
- The organism is present on the patient’s skin or has been shed onto objects in his environment.
- The organism is transmitted to the hands of health care worker.
- The organism must be able to survive for at least a few minutes.
- The organism is not removed from the healthcare worker’s hands because of no or inadequate hand hygiene.
- The health care worker’s contaminated hand comes into contact with another patient, another part of the same patient or an object that will come into contact with the patient.
From the above it becomes clear that to break the cycle of transmission of infections caregivers must clean their hands at different points of patient contact and also use the proper techniques and cleaning agents. It is important to keep in mind that organisms can also be transmitted by a gloved hand.
The World Health Organization describes five key moments for hand hygiene:
- before touching a patient
- before clean and aseptic procedures
- after contact with body fluids
- after touching a patient
- after touching patient surroundings.
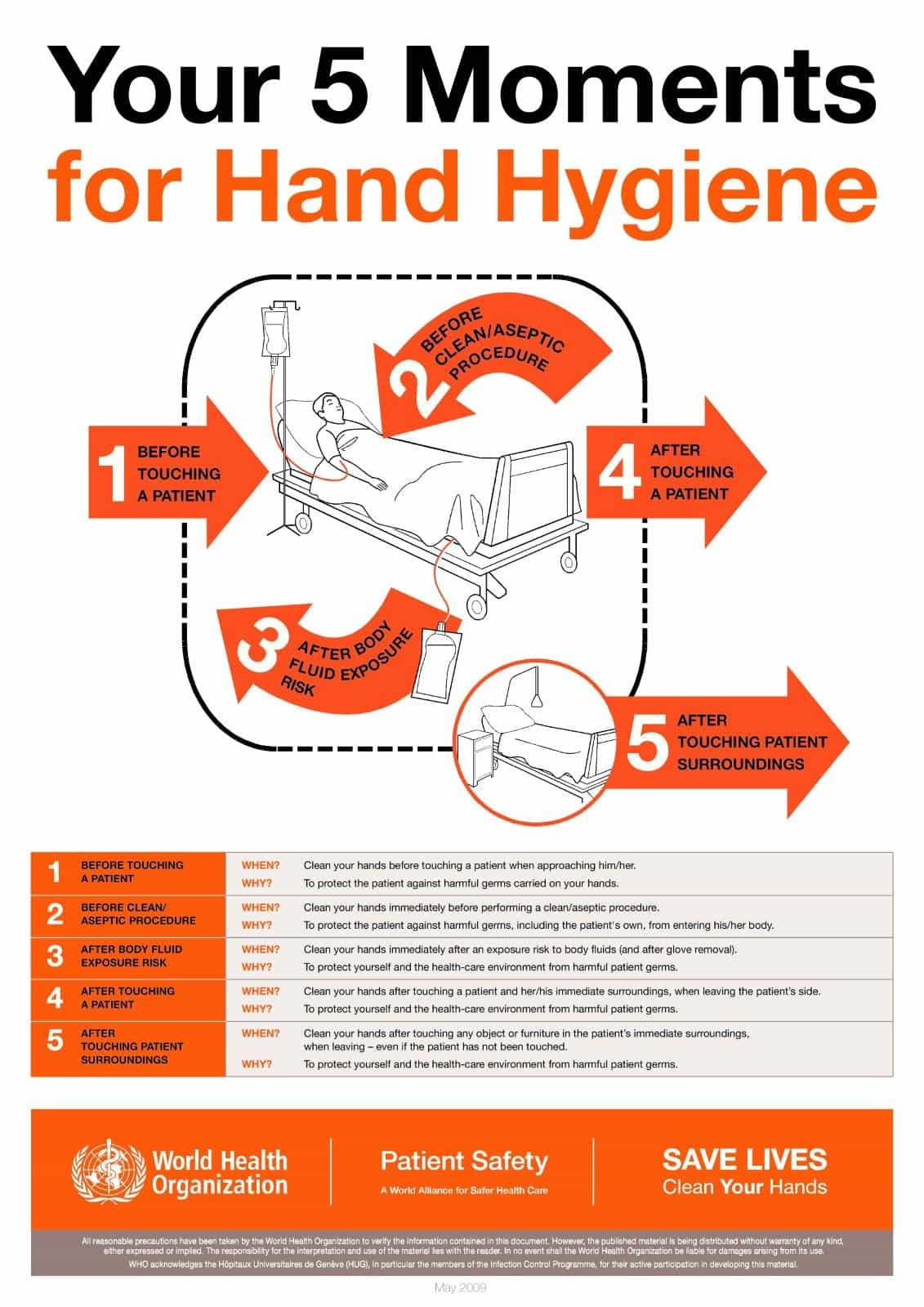
On careful analysis of the above moments, it becomes obvious that transmission of infection can also occur during a sequence of care for the same patient. For example, after you have inserted a catheter and touch the patient’s hand, face or even an object in his environment.
Also remember to clean your hands thoroughly at the start of your shift. Epidemics of HCAI have been traced to a pot of body cream in a nurse’s residence as well as a nurse’s cat.
Research is ongoing into the best methods and preparations for hand hygiene, and you should not hesitate to adopt new routines established in the setting where you work.
Why do healthcare workers neglect hand hygiene?
Studies have shown numerous reasons why hand hygiene is neglected, especially considering that during an eight-hour shift doctors and nurses working in ICU’s may have to clean or wash their hands as many as one hundred times.
A lack of training and not understanding how essential hand hygiene is can lead to disregard of this infection control measure. Too little knowledge of the risks of cross-infection and skepticism about the value of hand hygiene can lead to indifference to the protocols, not thinking about it or forgetting. Some may purposely skip the routine because of skin irritation and dryness.
Various organizational factors have also been associated lack of proper hand hygiene habits. One of the most significant is where hand hygiene is not prioritized and promoted through campaigns as well role modeling by senior staff. Understaffing and time pressure can also bring about the neglect of basic infection control measures. Even the availability, location and height of sinks as well as the shortage of cleaning agents and paper towels could be contributing factors.
We are human and with the numerous moments calling for hand hygiene during an 8-hour shift it is not surprising that health care workers cut corners. Whenever you are tempted to do so, remind yourself of the risks to the safety and well-being of your patients.


























Leave a Comment