Learn about the nursing care management of patients with asthma in this nursing study guide.
What is Asthma?
Asthma affects people in their different stages in life, yet it can be avoided and treated.
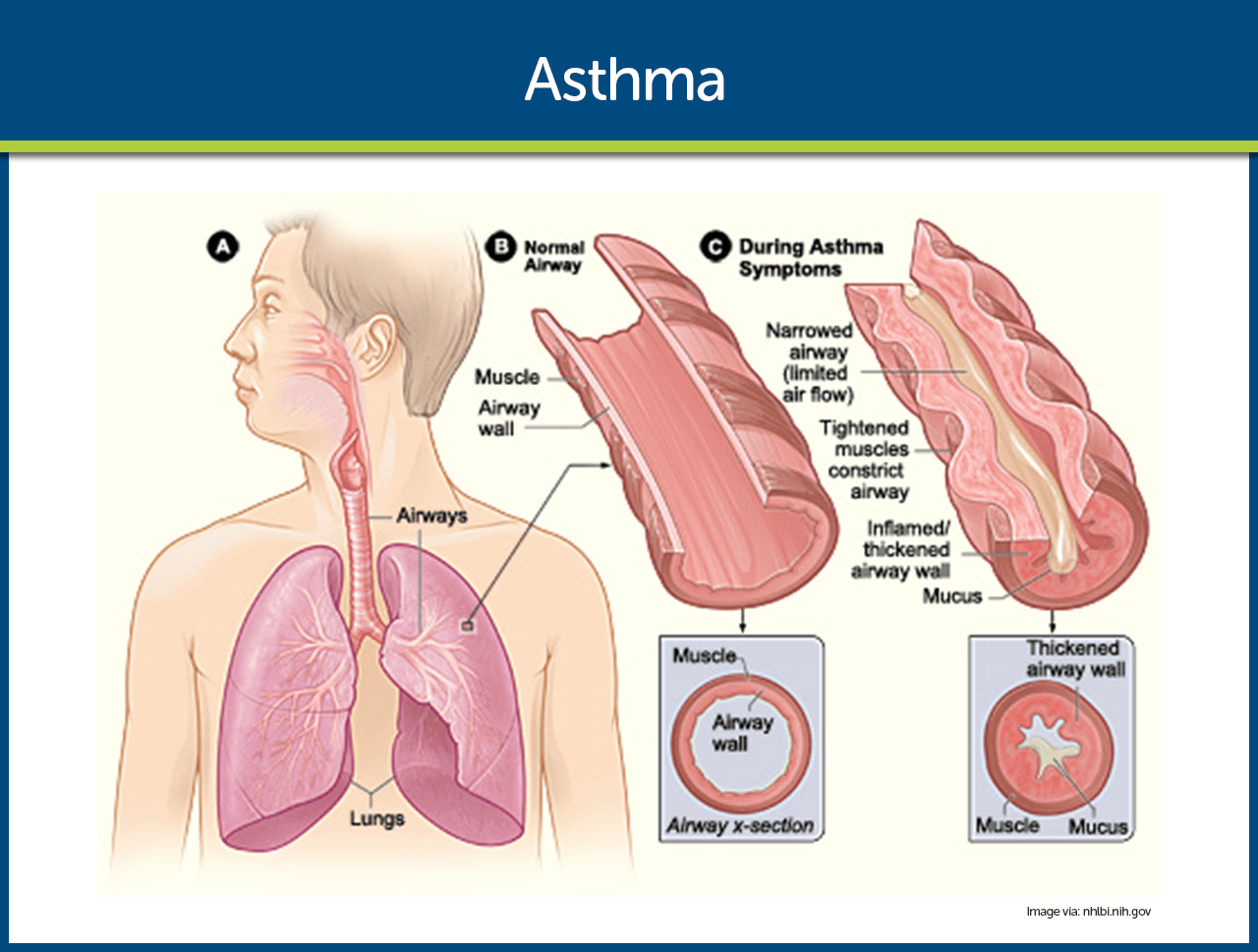
- Asthma is a chronic inflammatory disease of the airways that causes airway hyperresponsiveness, mucosal edema, and mucus production.
- Inflammation ultimately leads to recurrent episodes of asthma symptoms.
- Patients with asthma may experience symptom-free periods alternating with acute exacerbations that last from minutes to hours or days.
- Asthma, the most common chronic disease of childhood, can begin at any age.
Pathophysiology
The underlying pathophysiology in asthma is reversible and diffuse airway inflammation that leads to airway narrowing.
- Activation. When the mast cells are activated, it releases several chemicals called mediators.
- Perpetuation. These chemicals perpetuate the inflammatory response, causing increased blood flow, vasoconstriction,, fluid leak from the vasculature, the attraction of white blood cells to the area, and bronchoconstriction.
- Bronchoconstriction. Acute bronchoconstriction due to allergens results from a release of mediators from mast cells that directly contract the airway.
- Progression. As asthma becomes more persistent, the inflammation progresses and other factors may be involved in the airflow limitation.
Statistics and Epidemiology
Asthma is considered the most common chronic disease of childhood and is a disruptive disease that affects school and work attendance.
- Asthma affects more than 22 million people in the United States.
- Asthma accounts for more than 497, 000 hospitalizations annually.
- The total economic cost of asthma exceeds $27.6 billion.
Causes
Despite increased knowledge on the pathology of asthma and the development of improved medications and management plans, the death rate from the disease continues to rise. Here are some of the factors that influence the development of asthma.
- Allergy. Allergy is the strongest predisposing factor for asthma.
- Chronic exposure to airway irritants. Irritants can be seasonal (grass, tree, and weed pollens) or perennial (mold, dust, roaches, animal dander).
- Exercise. Too much exercise can also cause asthma.
- Stress/ Emotional upset. This can trigger constriction of the airway leading to asthma.
- Medications. Certain medications can trigger asthma.
Clinical Manifestations
The signs and symptoms of asthma can be easily identified, so once the following symptoms are observed, a visit to the physician is necessary.
- Most common symptoms of asthma are cough (with or without mucus production), dyspnea, and wheezing (first on expiration, then possibly during inspiration as well).
- Cough. There are instances that cough is the only symptom.
- Dyspnea. General tightness may occur which leads to dyspnea.
- Wheezing. There may be wheezing, first on expiration, and then possibly during inspiration as well.
- Asthma attacks frequently occur at night or in the early morning.
- An asthma exacerbation is frequently preceded by increasing symptoms over days, but it may begin abruptly.
- Expiration requires effort and becomes prolonged.
- As exacerbation progresses, central cyanosis secondary to severe hypoxia may occur.
- Additional symptoms, such as diaphoresis, tachycardia, and a widened pulse pressure, may occur.
- Exercise-induced asthma: maximal symptoms during exercise, absence of nocturnal symptoms, and sometimes only a description of a “choking” sensation during exercise.
- A severe, continuous reaction, status asthmaticus, may occur. It is life-threatening.
- Eczema, rashes, and temporary edema are allergic reactions that may be noted with asthma.
Prevention
Patients with recurrent asthma should undergo tests to identify the substances that precipitate the symptoms.
- Allergens. Allergens, either seasonal or perennial, can be prevented through avoiding contact with them whenever possible.
- Knowledge. Knowledge is the key to quality asthma care.
- Evaluation. Evaluation of impairment and risk are key in the control.
Complications
Complications for asthma include the following:
- Status asthmaticus. Airway obstruction in status asthmaticus often results in hypoxemia.
- Respiratory failure. Asthma, if left untreated, progresses to respiratory failure.
- Pneumonia. Mucus that pools in the lungs and becomes infected can lead to the development of pneumonia.
Assessment and Diagnostic Findings
To determine the diagnosis of asthma, the clinician must determine that episodic symptoms of airway obstruction are present.
- Positive family history. Asthma is a hereditary disease, and can be possibly acquired by any member of the family who has asthma within their clan.
- Environmental factors. Seasonal changes, high pollen counts, mold, pet dander, climate changes, and air pollution are primarily associated with asthma.
- Comorbid conditions. Comorbid conditions that may accompany asthma may include gastroeasophageal reflux, drug-induced asthma, and allergic broncopulmonary aspergillosis.
Medical Management
Immediate intervention may be necessary, because continuing and progressive dyspnea leads to increased anxiety, aggravating the situation.
Pharmacologic Therapy
- Short-acting beta2 –adrenergic agonists. These are the medications of choice for relief of acute symptoms and prevention of exercise-induced asthma.
- Anticholinergics. Anticholinergics inhibit muscarinic cholinergic receptors and reduce intrinsic vagal tone of the airway.
- Corticosteroids. Corticosteroids are most effective in alleviating symptoms, improving airway function, and decreasing peak flow variability.
- Leukotriene modifiers. Anti Leukotrienes are potent bronchoconstrictors that also dilate blood vessels and alter permeability.
- Immunomodulators. Prevent binding of IgE to the high affinity receptors of basophils and mast cells.
Peak Flow Monitoring

- Peak flow meters. Peak flow meters measure the highest airflow during a forced expiration.
- Daily peak flow monitoring. This is recommended for patients who meet one or more of the following criteria: have moderate or severe persistent asthma, have poor perception of changes in airflow or worsening symptoms, have unexplained response to environmental or occupational exposures, or at the discretion of the clinician or patient.
- Function. If peak flow monitoring is used, it helps measure asthma severity and, when added to symptom monitoring, indicates the current degree of asthma control.
Nursing Management
The immediate care of patients with asthma depends on the severity of the symptoms.
Nursing Assessment
Assessment of a patient with asthma includes the following:
- Assess the patient’s respiratory status by monitoring the severity of the symptoms.
- Assess for breath sounds.
- Assess the patient’s peak flow.
- Assess the level of oxygen saturation through the pulse oximeter.
- Monitor the patient’s vital signs.
Nursing Diagnosis
Based on the data gathered, the nursing diagnoses appropriate for the patient with asthma include:
- Ineffective airway clearance related to increased production of mucus and bronchospasm.
- Impaired gas exchange related to altered delivery of inspired O2.
- Anxiety related to perceived threat of death.
Nursing Care Planning & Goals
Main Article: 5 Bronchial Asthma Nursing Care Plans
To achieve success in the treatment of a patient with asthma, the following goals should be applied:
- Maintenance of airway patency.
- Expectoration of secretions.
- Demonstration of absence/reduction of congestion with breath sounds clear, respirations noiseless, improved oxygen exchange.
- Verbalization of understanding of causes and therapeutic management regimen.
- Demonstration of behaviors to improve or maintain clear airway.
- Identification of potential complications and how to initiate appropriate preventive or corrective actions.
Nursing Interventions
The nurse generally performs the following interventions:
- Assess history. Obtain a history of allergic reactions to medications before administering medications.
- Assess respiratory status. Assess the patient’s respiratory status by monitoring the severity of symptoms, breath sounds, peak flow, pulse oximetry, and vital signs.
- Assess medications. Identify medications that the patient is currently taking. Administer medications as prescribed and monitor the patient’s responses to those medications; medications may include an antibiotic if the patient has an underlying respiratory infection.
- Pharmacologic therapy. Administer medications as prescribed and monitor patient’s responses to medications.
- Fluid therapy. Administer fluids if the patient is dehydrated.
Evaluation
To determine the effectiveness of the plan of care, evaluation must be performed. The following must be evaluated:
- Maintenance of airway patency.
- Expectoration or clearance of secretions.
- Absence /reduction of congestion with breath sound clear, noiseless respirations, and improved oxygen exchange.
- Verbalized understanding of causes and therapeutic management regimen.
- Demonstrated behaviors to improve or maintain clear airway.
- Identified potential complications and how to initiate appropriate preventive or corrective actions.
Discharge and Home Care Guidelines
A major challenge is to implement basic asthma management principles at the home and community level.
- Collaboration. The complex therapy of treating asthma at home needs collaboration between the patient and the health care provider to determine the desired outcomes and to formulate a plan to achieve those outcomes.
- Health education. Patient teaching is a critical component of care for patients with asthma. Teach patient and family about asthma (chronic inflammatory), purpose and action of medications, triggers to avoid and how to do so, and proper inhalation technique. Instruct patient and family about peak-flow monitoring. Obtain current educational materials for the patient based on the patient’s diagnosis, causative factors, educational level, and cultural background.
- Compliance to therapy. Nurses should emphasize adherence to the prescribed therapy, preventive measures, and the need to keep follow-up appointments with health care providers. Teach patient how to implement an action plan and how and when to seek assistance.
- Home visits. Home visits by the nurse to assess the home environment for allergens may be indicated for patients with recurrent exacerbations.
Documentation Guidelines
Documentation is a necessary part of the nursing care provided, and the following data must be documented:
- Related factors for individual client.
- Breath sounds, presence and character of secretions, and use of accessory muscles for breathing.
- Character of cough and sputum.
- Respiratory rate, pulse oximetry/o2 saturation, and vital signs.
- Plan of care and who is involved in planning.
- Teaching plan.
- Client’s response to interventions, teaching, and actions performed.
- Use of respiratory devices/airway adjuncts.
- Response to medications administered.
- Attainment or progress towards desired outcomes.
- Modifications to the plan of care.
See Also
Posts related to Asthma:




























Leave a Comment