Placenta previa is a high-risk complication that occurs during pregnancy, affecting the positioning of the placenta in relation to the cervix. In this condition, the placenta partially or completely covers the cervical opening, leading to potential risks of severe bleeding during labor and delivery. Placenta previa requires vigilant monitoring, timely diagnosis, and appropriate management to ensure the safety and well-being of both the expectant mother and her unborn baby.
This article provides a concise overview of placenta previa, highlighting its implications, clinical manifestations, diagnostic methods, nursing interventions, and the importance of prompt medical intervention in mitigating potential complications.
What is Placenta Previa?
- Placenta previa is a pregnancy complication where the placenta partially or completely covers the opening of the cervix, impeding the normal pathway for childbirth. This condition can lead to vaginal bleeding, especially during the third trimester.
Pathophysiology
- The placenta implants on the lower part of the uterus.
- The lower uterine segment separates from the upper segment as the cervix starts to dilate.
- The placenta is unable to stretch and accommodate the shape of the cervix, resulting in bleeding.
Risk Factors
Placenta previa is dangerous if not detected early. However, it is also highly preventable once you get to know the risk factors.
- Advanced maternal age. Women who are over the age of 35 years old are at an increased risk of developing placenta previa.
- Multiple gestations. The uterus which has accommodated more than one fetus has an increased risk for placenta previa.
- Increased parity. Women who have given birth to a lot of children have an increased chance of having placenta previa.
- Past cesarean births. Giving birth via cesarean delivery predisposes the woman to placenta previa on her next childbearing.
- Past uterine curettage. Scars from a past curettage can affect the implantation of the uterus and lead to placenta previa.
Types
These types of placenta previa are classified according to the degree of the opening that is covered by the placenta.
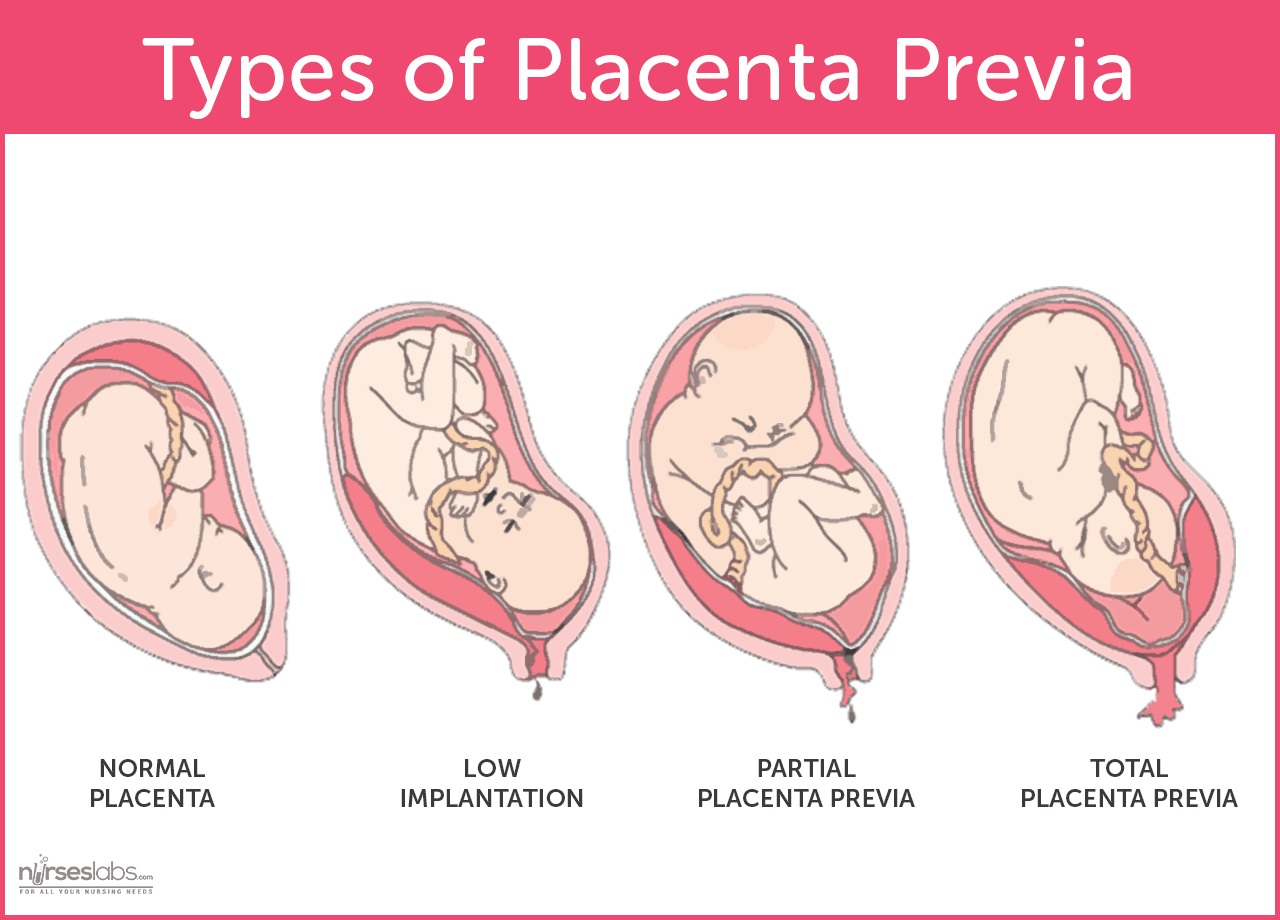
- Low lying placenta. The placenta implants in the lower portion instead of the upper portion of the uterus.
- Marginal implantation. The placenta’s edge is nearing the cervical os.
- Partial placenta previa. A portion of the cervical os is already covered by the placenta.
- Total placenta previa. The placenta occludes the entire cervical os.
Signs and Symptoms
The following signs and symptoms of placenta previa must be detected immediately by the health care providers to avoid risking the life of the fetus.
- Bright red bleeding. When the placenta is unable to stretch to accommodate the shape of the cervix, bleeding will occur suddenly which could frighten the woman.
- Painless. Bleeding in placenta previa is not painless and may also stop as abruptly as it had begun.
Diagnostic Tests
To diagnose placenta previa, the patient must undergo the following diagnostic procedure.
- Ultrasound. Early detection of placenta previa is always possible through ultrasonography. It is the most common and initial diagnostic test that could confirm the diagnosis.
Medical Management
Medical interventions are necessary to ensure that the safety of both mother and fetus are still intact.
- Intravenous therapy. This would be prescribed by the physician to replace the blood that was lost during bleeding.
- Avoid vaginal examinations. This may initiate hemorrhage that is fatal for both the mother and the baby.
- Attach external monitoring equipment. To monitor the uterine contractions and record fetal heart sounds, external equipment is preferred to internal monitoring equipment.
Surgical Management
Surgical interventions are carried out once the condition of both the mother and the fetus has reached a critical stage and their lives are exposed to undeniable danger.
- Cesarean delivery. Although the best way to deliver a baby is through normal delivery, if the placenta has obstructed more than 30% of the cervical os it would be hard for the fetus to get past the placenta through normal delivery. Cesarean birth is then recommended by the physician.
Nursing Management
Nurses also play a major role in the care of a woman with placenta previa. They are also entrusted with the outcome of the lives of both the mother and the child.
Nursing Assessment
- Assess baseline vital signs, especially blood pressure. The physician would order monitoring of the blood pressure every 5-15 minutes.
- Assess fetal heart sounds to monitor the well-being of the fetus.
- Monitor uterine contractions to establish the progress of labor of the mother.
- Weigh perineal pads used during bleeding to calculate the amount of blood lost.
- Assist the woman in a side-lying position when bleeding occurs.
Nursing Diagnosis
Nursing Care Plans
Main article: Placenta Previa Nursing Care Plans
For more nursing care plans, please visit our Nursing Care Plan page.
Nursing Interventions
- Assess fetal heart sounds so the mother would be aware of the health of her baby.
- Allow the mother to vent her feelings to lessen her emotional stress.
- Assess any bleeding or spotting that might occur to give adequate measures.
- Answer the mother’s questions honestly to establish a trusting environment.
- Include the mother in the planning of the care plan for both the mother and the baby.
Evaluation
- The woman is able to discuss her concerns with the healthcare providers.
- States that hearing the fetal heartbeat assures her of the baby’s safety.
One could move mountains just to save the lives of their mother and child. That is also true for health care providers. The conditions that affect the health of the mother and the baby can be conquered if both the support system and the health care providers are working as a team towards one measurable purpose: to save lives.




























Leave a Comment