Abruptio placentae, also known as placental abruption, is a critical obstetric emergency characterized by the premature detachment of the placenta from the uterine wall before childbirth. This serious condition can result in significant maternal hemorrhage and jeopardize the well-being of the fetus. Early recognition, timely intervention, and skilled nursing care are essential in lessening the potential complications of abruptio placentae, ensuring the best possible outcomes for both the mother and the baby.
This nursing note provides a brief overview of this pregnancy complication, highlighting its significance in obstetrics and the crucial role of nursing in managing such cases effectively.
What is Abruptio Placentae?
- Abruptio placentae (also known as placental abruption) is the premature separation of the placenta that occurs late in the pregnancy.
Pathophysiology
- The placenta has been implanted in the correct location.
- For some unknown reason, it suddenly begins to separate, causing bleeding.
- This separation would occur late in pregnancy and accounts for 10% of perinatal deaths.
Risk Factors
The following are the risk factors that surround abruptio placenta and these should be made known to all pregnant mothers to avoid the development of this fatal condition.
- High parity. A woman who has given birth multiple times predisposes herself to abruptio placentae.
- Short umbilical cord. A short umbilical cord could cause the separation of the placenta especially if trauma occurs.
- Advanced maternal age. Women over the age of 35 years old have a higher risk of acquiring abruptio placentae.
- Direct trauma. Any trauma to the abdomen could cause a separation of the placenta.
- Chorioamnionitis. This is an infection of the fetal membranes and fluid that could predispose the woman to premature placental separation.
Types
The types of abruption placenta are measured according to the degree of placental separation that has occurred.
- Grade 0. No indication of placental separation and diagnosis of slight separation is made after birth.
- Grade 1. There is minimal separation which causes vaginal bleeding, but no changes in fetal vital signs occur.
- Grade 2. Moderate separation occurs and fetal distress is already evident. The uterus is also hard and painful upon palpation.
- Grade 3. Extreme separation; maternal shock and fetal death is imminent if no interventions are done.
Signs and Symptoms
The signs and symptoms of abruption placenta must be monitored and detected early before it progresses to a critical stage.
- Sharp, stabbing pain. A woman may experience pain in the upper uterine fundus as initial separation occurs.
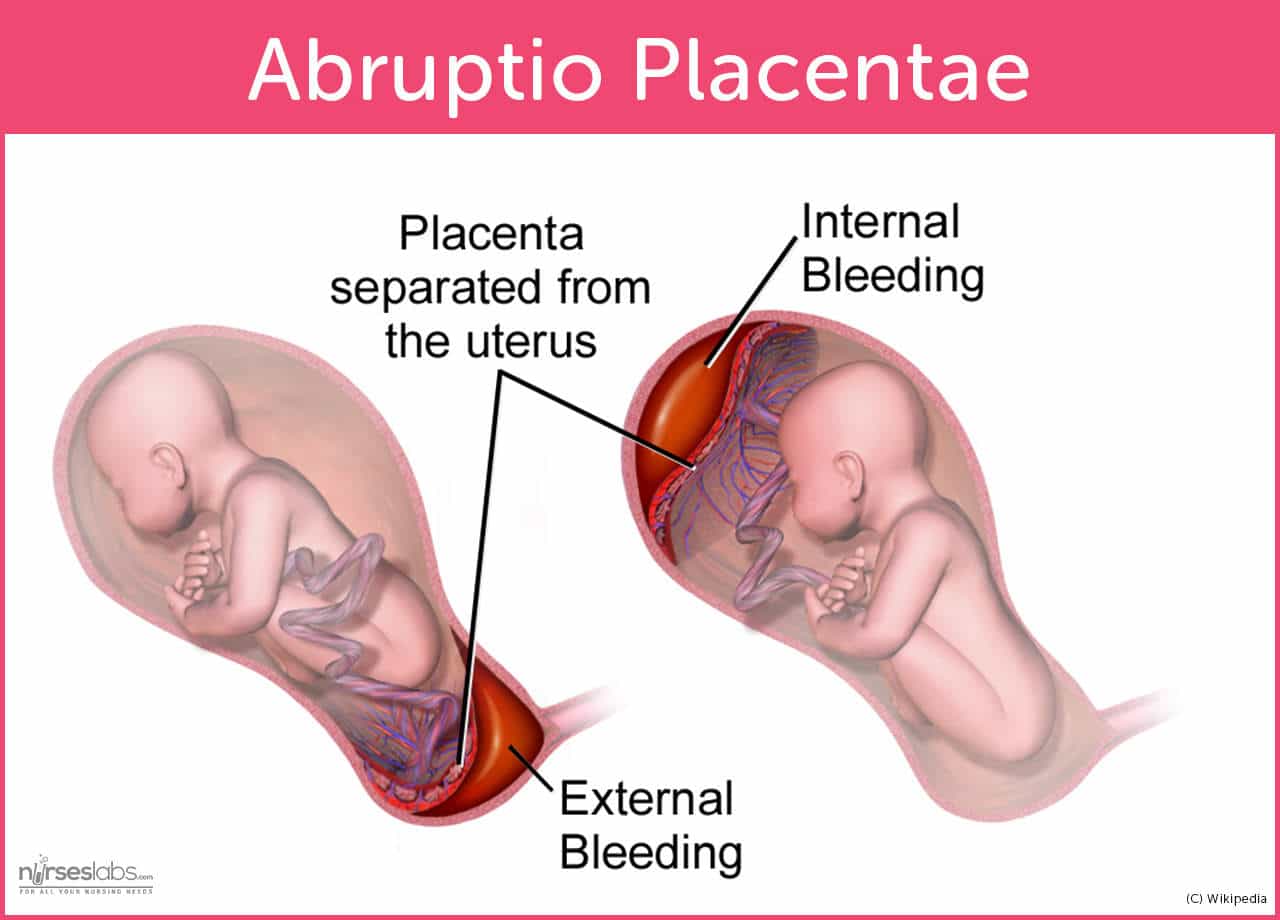
- Heavy bleeding. This usually happens after the separation of the placenta. External bleeding will only occur if the placenta separates first from the edges. Internal bleeding will occur if the placenta separates from the center because blood would pool under it.
- The uterus is tense and rigid. Most often called as Couvelaire uterus, it appears as a board-like, hard uterus without any bleeding.
Diagnostic Tests
These diagnostic procedures would be enforced by the physician to finally diagnose the presence of abruptio placenta.
- Hemoglobin level and fibrinogen level. These tests are performed to rule out disseminated intravascular coagulation.
Medical Management
To avoid a worsening condition, these medical procedures are implemented for both the mother and the fetus.
- Intravenous therapy. Once the woman starts to bleed, the physician would order a large gauge catheter to replace the fluid losses.
- Oxygen inhalation. Delivered via face mask, this would prevent fetal anoxia.
- Fibrinogen determination. This test would be taken several times before birth to detect DIC.
Surgical Management
Once the condition has reached a stage that mightily endangers the life of both patients, then surgical management is put into action.
- Cesarean delivery. If birth is imminent, it is safest to deliver the baby via cesarean delivery.
- Hysterectomy. The worst outcome would be for the woman to develop DIC, and to prevent exsanguinations, a hysterectomy must be performed.
Nursing Management
A vital role is also upheld by the nurses during this situation. Their accurate assessment would be one of the baseline data for all healthcare providers to plot the care plan for the patient.
Nursing Assessment
- Assess for signs of shock, especially when heavy bleeding occurs.
- Assess if the bleeding is external or internal.
- Monitor contractions if separation occurs during labor.
- Obtain baseline vital signs.
- Assess the time the bleeding began, the amount and kind of bleeding, and interventions done when bleeding occurred if it started before admission.
- Assess for the quality of pain.
Nursing Diagnosis
- Deficient fluid volume related to bleeding during premature placental separation.
Nursing Care Plans
- Check out our Nursing Care Plans page.
Nursing Interventions
- Place the woman in a lateral, not supine position to avoid pressure in the vena cava.
- Monitor fetal heart sounds.
- Monitor maternal vital signs to establish baseline data.
- Avoid performing any vaginal or abdominal examinations to prevent further injury to the placenta.
Evaluation
- Maternal vital signs are all within the normal range, especially blood pressure.
- Urine output should be more than 30mL/hr.
- No bleeding or minimal amount of bleeding was observed.
- Uterus is not tense and rigid.
- Fetal heart sounds are within the normal range.
The team of health care providers could very well be the key towards the survival and safety of both the mother and the fetus. The role of the support system is also essential for this situation. Finally, the willpower of the mother to survive with both of their lives intact could be the turning point for those who care deeply for the patient and the child.




























Leave a Comment