Tonsillitis and adenoiditis are common inflammatory conditions affecting the tonsils and adenoids, respectively, often encountered in pediatric and adult populations. As nursing professionals, understanding the nuances of these conditions and providing effective management and relief is vital in ensuring the well-being of patients experiencing the discomfort and potential complications associated with these infections.
This article aims to serve as a comprehensive nursing guide to tonsillitis and adenoiditis, delving into their etiology, clinical manifestations, diagnostic methods, and evidence-based interventions.
What is Tonsillitis?
The consideration of quinsy in the differential diagnosis of George Washington’s death and the discussion of tonsillitis in Kean’s Domestic Medical Lectures, a home medical companion book published in the late 19th century, reflect the rise of tonsillitis as a medical concern.
- Tonsillitis is a common illness in childhood resulting from pharyngitis.
- Tonsillitis is the inflammation of the pharyngeal tonsils; the inflammation usually extends to the adenoid and the lingual tonsils.
Pathophysiology
A brief description of the location and functions of the tonsils and adenoids serves as an introduction to the discussion of their infection and medical and surgical treatments.
- A ring of lymphoid tissue encircles the pharynx, forming a protective barrier against upper respiratory infection.
- This ring consists of groups of lymphoid tonsils, including the faucial, the commonly known tonsils; pharyngeal, known as adenoids; and lingual tonsils.
- Lymphoid tissue normally enlarges progressively in childhood between the ages of 2 and 10 years and shrinks during preadolescence.
- If the tissue itself becomes a site of acute or chronic infection, it may become hypertrophied and can interfere with breathing, may cause partial deafness, or may become a source of infection in itself.
Statistics and Incidences
Tonsillitis most often occur in children; however, the condition rarely occurs in children younger than 2 years.
- Recurrent tonsillitis was reported in 11.7% of Norwegian children in one study and estimated in another study to affect 12.1% of Turkish children.
- In one study, the mean prevalence of carrier status of schoolchildren for group A Streptococcus, a cause of tonsillitis, was 15.9%.
- According to Herzon et al, children account for approximately one-third of peritonsillar abscess episodes in the United States.
- Klug found seasonal and/or age-based variations in the incidence and cause of tonsillitis.
- Among his conclusions, he reported that the incidence of tonsillitis increased during childhood, peaking in teenagers and then gradually falling until old age.
- He also found that until age 14 years, girls were more affected than boys, but that the condition subsequently was more frequent in males than in females.
Causes
Viral or bacterial infections and immunologic factors lead to tonsillitis and its complications.
- Epstein-Barr virus (EBV). In one study showing that EBV may cause tonsillitis in the absence of systemic mononucleosis, EBV was found to be responsible for 19% of exudative tonsillitis in children.
- Bacteria. Anaerobic bacteria play an important role in tonsillar disease; most cases of bacterial tonsillitis are caused by group A beta-hemolytic Streptococcus pyogenes (GABHS); S. pyogenes adheres to adhesin receptors that are located on the tonsillar epithelium; immunoglobulin coating of pathogens may be important in the initial induction of bacterial tonsillitis.
- Immunologic. Local immunologic mechanisms are important in chronic tonsillitis; the distribution of dendritic cells and antigen-presenting cells is altered during disease, with fewer dendritic cells on the surface epithelium and more in the crypts and extrafollicular areas.
Clinical Manifestations
The child with tonsillitis may exhibit the following signs and symptoms:
- Fever. The child may present with a fever of 101°F (38.4°C) or more.
- Sore throat. The child may also manifest a sore throat, often with dysphagia or difficulty swallowing.
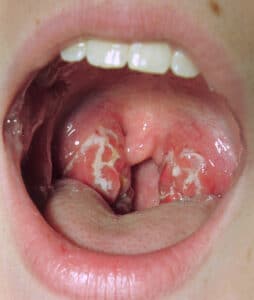
- Hypertrophied tonsils. Individuals with acute tonsillitis present with tender and inflamed tonsils; exudate may also be visible on the tonsils.
- Airway obstruction. Airway obstruction may manifest as mouth breathing, snoring, sleep-disordered breathing, nocturnal breathing pauses, or sleep apnea.
Assessment and Diagnostic Findings
Testing is indicated when group A beta-hemolytic Streptococcus pyogenes (GABHS) infection is suspected.
- Throat cultures. Throat cultures are performed to diagnose tonsillitis and the causative organism.
- Imaging studies. For patients in whom acute tonsillitis is suspected to have spread to deep neck structures (ie, beyond the fascial planes of the oropharynx), radiologic imaging using plain films of the lateral neck or CT scans with contrast is warranted.
Medical Management
Treatment of acute tonsillitis is largely supportive and focuses on maintaining adequate hydration and caloric intake and controlling pain and fever.
- Hydration. Inability to maintain adequate oral caloric and fluid intake may require IV hydration, antibiotics, and pain control; home intravenous therapy under the supervision of qualified home health providers or the independent oral intake ability of patients ensures hydration; intravenous corticosteroids may be administered to reduce pharyngeal edema.
- Management of airway obstruction. Airway obstruction may require management by placing a nasal airway device, using intravenous corticosteroids, and administering humidified oxygen; observe the patient in a monitored setting until the airway obstruction is clearly resolving.
- Tonsillectomy. Tonsillectomy is indicated for individuals who have experienced more than six (6) episodes of streptococcal pharyngitis (confirmed by positive culture) in 1 year, 5 episodes in 2 consecutive years, or 3 or more infections of tonsils and/or adenoids per year for 3 years in a row despite adequate medical therapy, or chronic or recurrent tonsillitis associated with the streptococcal carrier state that has not responded to beta-lactamase–resistant antibiotics.
- Adenoidectomy. Because adenoid tissue has similar bacteriology to the pharyngeal tonsils and because minimal additional morbidity occurs with adenoidectomy if tonsillectomy is already being performed, most surgeons perform an adenoidectomy if adenoids are present and inflamed at the time of tonsillectomy.
- Diet. Hydration is important, and the oral route is usually adequate.
- Activity. Adequate rest for children with tonsillitis accelerates recovery.
Pharmacologic Management
Medications that are used to manage tonsillitis include antibiotics, anti-inflammatory agents (e.g., corticosteroids), antipyretics and analgesics (e.g., acetaminophen, ibuprofen), and immunologic agents (e.g., gamma globulin).
- Corticosteroids. Corticosteroids have anti-inflammatory properties and cause profound and varied metabolic effects; these agents modify the body’s immune response to diverse stimuli; corticosteroids reduce inflammation, which may impair swallowing and breathing.
- Antibiotics. Antibiotic therapy must be comprehensive and cover all likely pathogens in the context of this clinical setting.
- Immune globulins. These agents are used to improve clinical aspects of the disease; it stimulates immune cells, reducing the severity of infection.
- Analgesics. Pain and fever control are essential to quality patient care; analgesics with antipyretic properties ensure patient comfort, promote pulmonary toilet, and have sedating properties, which are beneficial for patients who experience pain.
Nursing Management
Nursing treatment of tonsillitis consists of:
Nursing Assessment
Assessment of the child with tonsillitis includes:
- Preadmission assessment. Much of the preoperative operations, including laboratory studies, is done on a preadmission outpatient basis.
- History. Ask about any bleeding tendencies because postoperative bleeding is a concern.
- Vital signs. Take and record vital signs to establish a baseline for postoperative monitoring; the temperature is an important part of the data collection to determine that the child has no upper respiratory infection.
Nursing Diagnoses
Based on the assessment data, the major nursing diagnoses are:
- Risk for aspiration related to impaired swallowing and bleeding at the operative site.
- Acute pain related to inflammation of tonsils and the surgical procedure.
- Deficient fluid volume related to inadequate oral intake secondary to painful swallowing.
- Deficient knowledge related to caregivers understanding of postdischarge home care and signs and symptoms of complications.
Nursing Care Planning and Goals
Main Article: 4 Tonsillitis Nursing Care Plans
The major nursing care planning goals for a child with tonsillitis include:
- Preventing aspiration.
- Relieving pain, especially while swallowing.
- Improving fluid intake.
- Increase knowledge and understanding of postdischarge care and possible complications.
Nursing Interventions
Interventions for the child are:
- Prevent aspiration. Place the child in a partially prone position with head turned to one side until the child is completely awake; encourage the child to expectorate all secretions; discourage the child from coughing; and keep the head slightly lower than the chest to help facilitate drainage of secretions.
- Relieve pain. Apply an ice collar postoperatively; administer pain medication as ordered; encourage the caregiver to remain at the bedside to provide soothing reassurance; crying irritates the raw throat and increases the child’s discomfort; thus, it should be avoided if possible.
- Encourage fluid intake. When the child is fully awake from surgery, give small amounts of clear fluids or ice chips; avoid irritating liquids such as orange juice and lemonade; milk and ice cream products tend to cling to the surgical site and make swallowing more difficult; thus they are poor choices; and record intake and output until adequate oral intake is established.
- Provide family teaching. Instruct the caregiver to keep the child relatively quiet for a few days after discharge; recommend giving soft foods and nonirritating liquids for the first few days; teach family members to note any signs of hemorrhage and notify the healthcare provider; and provide written instructions and telephone numbers before discharge.
Evaluation
Goals are met as evidenced by:
- Prevention of aspiration.
- Relief from pain, especially while swallowing.
- Improvement of fluid intake.
- Increase of knowledge and understanding of postdischarge care and possible complications.
Documentation Guidelines
Documentation in a child with tonsillitis include:
- Individual findings, including recent antibiotic therapy and upper respiratory infections.
- Current antibiotic therapy.
- Cultural and religious beliefs, and expectations.
- Plan of care.
- Teaching plan.
- Responses to interventions, teaching, and actions performed.
- Postoperative care.
- Modifications to the plan of care.
- Attainment or progress toward desired outcomes.




























Leave a Comment