The most common facial malformations, cleft lip and cleft palate, occur either alone or in combination.
Cleft lip and cleft palate are congenital anomalies that occur during early fetal development, resulting in a gap or opening in the upper lip and/or the roof of the mouth (palate). These common birth defects can vary in severity and have significant implications for speech, feeding, and facial structure.
Cleft lip and cleft palate can be emotionally challenging for affected individuals and their families, necessitating comprehensive and multidisciplinary care from healthcare professionals.
What is Cleft Lip and Cleft Palate?
Cleft lip and cleft palate are openings or splits in the upper lip, the roof of the mouth (palate), or both. Although both conditions can often appear together, either defect may appear alone.
- Cleft lip is a condition where there is a gap or split in the upper lip, often extending upward toward the nose. This gap can be small or extensive and may occur on one or both sides of the lip.
- Cleft palate, on the other hand, is a condition where there is an opening or gap in the roof of the mouth (palate). This gap may extend from the front of the mouth toward the back, and it can vary in size and severity.
Pathophysiology
In embryonic development, the palate closes later than the lip, and the failure to close occurs for different reasons.
- The cleft lip and palate defects result from failure of the maxillary and premaxillary processes to fuse during the 5th to 8th week of intrauterine life.
- The cleft may be a simple notch in the vermilion line, or it may extend up into the floor of the nose.
- The child born with a cleft palate but with an intact lip does not have the external disfigurement that may be so distressing to the new parent; however, the problems are more serious.
- In an 8-week old embryo, there is still no roof to the mouth; the tissues that are to become the palate are two shelves running from the front to the back of the mouth and projecting vertically downward on either side of the tongue.
- The shelves move from a vertical position to a horizontal position; their free edges meet and fuse in the midline.
- Later, bone forms within this tissue to form the hard palate.
- Normally the palate is intact by the 10th week of fetal life.
- Exactly what happens to prevent this closure is not known for sure, leading to a cleft lip and cleft palate.
Statistics and Incidences
Parents and family are naturally eager to see and hold their newborn and must be prepared for the shock of seeing the facial disfigurement.
- Cleft lip occurs in about 1 in 1,000 live births and is more common in males.
- Cleft palate occurs in 1 newborn in 2, 500, more often in females.
- Cleft palate occurs with a cleft lip about 50% of the time, most often with bilateral cleft lip.
Causes
The incidence of cleft palate is higher in the close relatives of people with the defect than it is in the general population, and some evidence indicates that environmental and hereditary factors play a part in this defect.
- Hereditary. The mother or the father can pass on genes that cause clefting, either alone or as part of a genetic syndrome that includes a cleft lip or cleft palate as one of its signs.
- Environmental. In some cases, babies inherit a gene that makes them more likely to develop a cleft, and then an environmental trigger actually causes the cleft to occur.
Clinical Manifestations
Usually, a split (cleft) in the lip or palate is immediately identifiable at birth.

- Cleft. A split in the lip and roof of the mouth (palate) that can affect one or both sides of the face; a split in the lip that can appear as only a small notch in the lip or can extend from the lip through the upper gum and palate into the bottom of the nose; a split in the roof of the mouth that doesn’t affect the appearance of the face.
- Difficulty with feedings. The newborn easily becomes choked on liquids.
- Difficulty swallowing. The newborn has a hard time in swallowing, with potential for liquids or foods to come out the nose.
- Nasal speaking voice. Due to the split in the palate, the newborn has a nasal speaking voice.
Assessment and Diagnostic Findings
The physical appearance of the newborn confirms the diagnosis of cleft lip; diagnosis of cleft palate is made at birth.
- Inspection. Diagnosis of cleft palate is made at birth with the close inspection of the newborn’s palate; to be certain that a cleft palate is not missed, the examiner must insert a gloved finger into the newborn’s mouth to feel the palate to determine that it is intact.
- Observation. Cleft lip can be diagnosed through observation of the physical appearance of the newborn.
Medical Management
Treatment for a newborn with cleft lip and palate includes:
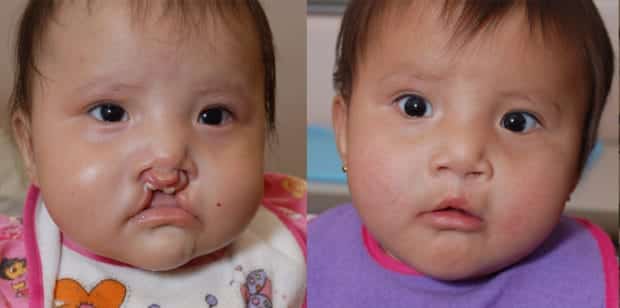
- Surgery. Cleft lip repair, usually performed by a plastic surgeon, is a major part of the treatment of a newborn with cleft lip, palate, or both; some surgeons favor early repair, before the newborn is discharged from the hospital; other surgeons prefer to wait until the newborn is 1 to 2 months old, weighs about 10 lbs, and is gaining weight steadily.
- Dental speech appliance. If surgery must be delayed beyond the 3rd year, a dental speech appliance may help aid the child develop intelligible speech.
Nursing Management
A complete and thorough process of care should be undergone by the newborn with cleft lip and cleft palate.
Nursing Assessment
One primary concern in the nursing care of a newborn with a cleft lip and cleft palate is the emotional care of the newborn’s family.
- Interview. In interviewing the family and collecting data, the nurse must include an exploration of the family’s acceptance of the newborn; conduct a thorough interview with the caregiver that includes a question about the methods they found to be most effective in feeding the infant.
- Physical exam. Physical examination of the infant includes temperature, apical pulse, and respirations; listening to breath sounds, observing skin turgor and color, infant’s neurologic status, noting alertness and responsiveness.
Nursing Diagnoses
Based on the assessment data, the major nursing diagnoses are:
- Compromised family coping related to visible physical defect.
- Anxiety of family caregivers related to child’s condition and surgical outcome.
- Deficient knowledge of family caregivers related to care of child before surgery and the surgical procedure.
- Risk for aspiration related to a reduced level of consciousness after surgery.
- Ineffective breathing pattern related to anatomical changes.
- Risk for deficient fluid volume related to NPO status after surgery.
- Acute pain related to surgical procedure.
- Risk of injury to the operative site related to newborn’s desire to suck thumb or fingers and anatomical changes.
Nursing Care Planning and Goals
Goal setting and planning must be modified to adapt to the surgical plans; the major goals include:
- Maintaining adequate nutrition.
- Increasing family coping.
- Reducing the parents’ anxiety and guilt regarding the newborn’s physical defects, and preparing parents for the future repair of the cleft lip and palate.
Nursing Interventions
Nursing interventions for the patient with cleft lip and palate are:
- Maintain adequate nutrition. Breastfeeding may be successful because the breast tissue may mold to close the gap; if the newborn cannot be breastfed, the mother’s breast milk may be expressed and used instead of formula; a soft nipple with a cross-cut made to promote easy flow of milk may work well.
- Positioning. If the cleft lip is unilateral, the nipple should be aimed at the unaffected side; the infant should be kept in an upright position during feeding.
- Tools for feeding. Lamb’s nipples (extra long nipples) and special cleft palate nipples molded to fit into the open palate area to close the gap may be used; one of the simplest and most effective methods may be the use of an eyedropper or an Asepto syringe with a short piece of rubber tubing on the tip (Breck feeder).
- Promote family coping. Encourage the family to verbalize their feelings regarding the defect and their disappointment; serve as a model for the family caregiver’s attitudes toward the child.
- Reduce family anxiety. Give the family information about cleft repairs; encourage them to ask questions and reassure them that any question is valid.
- Provide family teaching. Explain the usual routine of preoperative, intraoperative, and post-operative care; written information is helpful, but be certain the parents understand the information.
Evaluation
Major goals for the care of the infant with cleft lip and cleft palate include:
- Maintained adequate nutrition.
- Increased family coping.
- Reduced parents’ anxiety and guilt regarding the newborn’s physical defects.
Documentation Guidelines
Documentation for a patient with cleft lip and palate includes the following:
- Assessment findings, including current and past coping behaviors, emotional response to situation and stressors, and support systems available.
- Level of anxiety and precipitating/aggravating factors.
- Description of feelings.
- Awareness and ability to recognize and express feelings.
- Client’s description of the response to pain, specifics of pain inventory, and acceptable level of pain.
- Plan of care.
- Teaching plan.
- Responses of family members/client to interventions, teaching, and actions performed.
- Attainment or progress toward desired outcomes.
- Modification to plan of care.
- Long-term plan and who is responsible for actions.
- Specific referrals made.




























Leave a Comment