Idiopathic Thrombocytopenic Purpura (ITP) is a significant hematologic condition, that affects platelet levels in the blood, leading to potential bleeding and purpura formation. This autoimmune disorder arises from an immune system dysfunction, which mistakenly attacks and destroys platelets, critical components for clotting.
Understanding the complexities of ITP is vital for nurses in providing appropriate management and support to individuals living with this condition.
What is Idiopathic Thrombocytopenic Purpura?
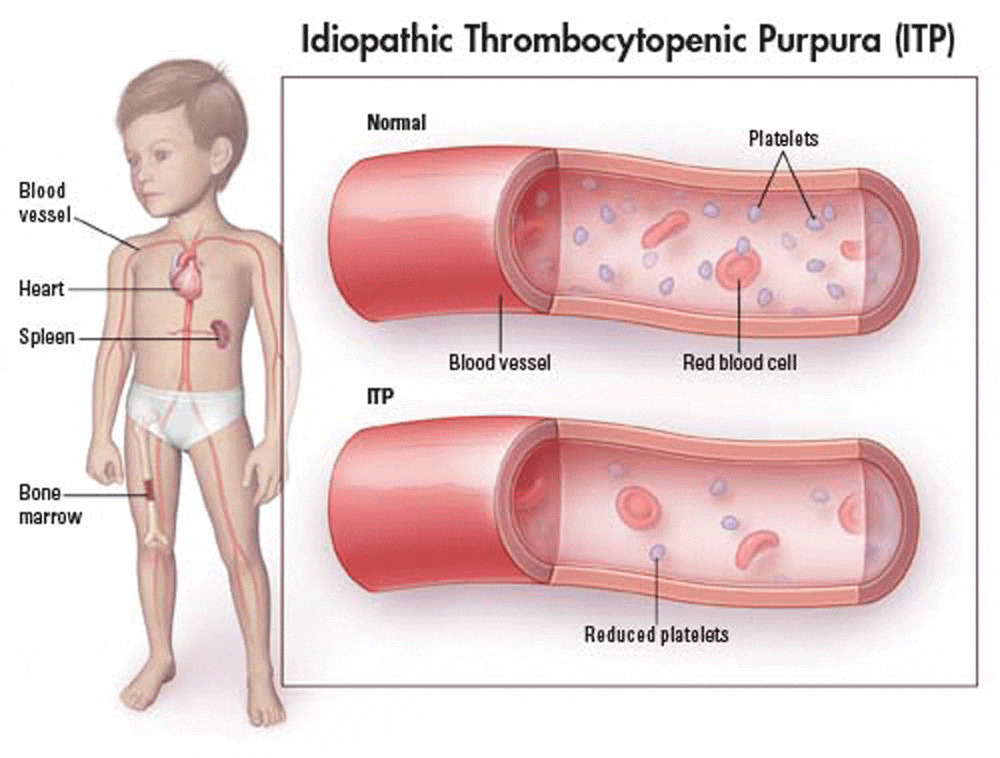
- Idiopathic thrombocytopenic purpura (ITP), also known as primary immune thrombocytopenic purpura and autoimmune thrombocytopenic purpura, is defined as isolated thrombocytopenia with normal bone marrow and in the absence of other causes of thrombocytopenia.
- ITP is a disorder that can lead to easy or excessive bruising and bleeding.
- Children often develop ITP after a viral infection and usually recover fully without treatment.
Pathophysiology
The bleeding results from unusually low levels of platelets — the cells that help blood clot.
- ITP is primarily a disease of increased peripheral platelet destruction, with most patients having antibodies to specific platelet membrane glycoproteins.
- Relative marrow failure may contribute to this condition since studies show that most patients have either normal or diminished platelet production.
- Acute ITP often follows an acute infection and has a spontaneous resolution within 2 months.
- Chronic ITP persists longer than 6 months without a specific cause.
Statistics and Incidences
Incidence rates of idiopathic thrombocytopenic purpura (ITP) are as follows:
- An average estimate of the incidence in children is 50 cases per 1,000,000 per year.
- New cases of chronic refractory ITP comprise approximately 10 cases per 1,000,000 per year
- According to studies in Denmark and England, childhood ITP occurs in approximately 10-40 cases per 1,000,000 per year.
- A prospective, population-based study in Norway indicated an incidence of 53 per 1,000,000 in children younger than 15 years.
- A study in Kuwait reported a higher incidence of 125 cases per 1,000,000 per year.
- The mortality rate from hemorrhage is approximately 1% in children and 5% in adults.
- Spontaneous remission occurs in more than 80% of cases in children.
- Peak prevalence occurs in children aged 2-4 years.
- Approximately 40% of all patients are younger than 10 years.
- In acute ITP (children), distribution is equal between males (52%) and females (48%).
Causes
If the cause of this immune reaction is unknown, the condition is called idiopathic thrombocytopenic purpura. Idiopathic means “of unknown cause.”
- Increased breakdown of platelets. In people with ITP, antibodies produced by the immune system attach themselves to the platelets, marking the platelets for destruction; the spleen, which helps the body fight infection, recognizes the antibodies and removes the platelets from the system; the result of this case of mistaken identity is a lower number of circulating platelets than is normal.
Clinical Manifestations
Clinical features of idiopathic thrombocytopenic purpura (ITP):
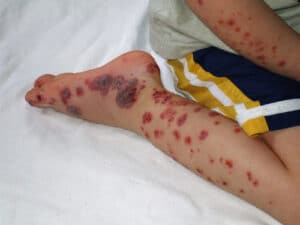
- Petechiae. Petechiae appear when capillaries bleed, leaking blood into the skin.
- Purpura. Easy or excessive bruising or purpura is dominant; if bone marrow megakaryocytes cannot increase production and maintain a normal number of circulating platelets, thrombocytopenia and purpura develop.
- Hemorrhage. Hemorrhagic bullae on mucous membranes, gingival bleeding, signs of GI bleeding, retinal hemorrhages, and evidence of intracranial hemorrhage, with possible neurologic symptoms; the bleeding results from unusually low levels of platelets — the cells that help blood clot.
- Nonpalpable spleen. The prevalence of palpable spleen in patients with ITP is approximately the same as that in the non-ITP population (ie, 3% in adults, 12% in children); despite the destruction of platelets by splenic macrophages, the spleen is normally not enlarged.
- Spontaneous bleeding. Spontaneous bleeding occur when platelet count is less than 20,000/mm3.
Assessment and Diagnostic Findings
Diagnosis of idiopathic thrombocytopenic purpura includes:
- Laboratory studies. Isolated thrombocytopenia on a complete blood cell count (CBC) is the key laboratory finding; the white blood cell (WBC) count and hemoglobin level typically are normal, unless severe hemorrhage has occurred; on peripheral smear, truly giant platelets suggest congenital thrombocytopenia.
- Imaging studies. A CT scan of the head is warranted if concern exists regarding intracranial hemorrhage.
Medical Management
Treatment may include a number of approaches, such as medications to boost platelet count or surgery to remove spleen (splenectomy).
- Prehospital care. Prehospital care focuses on the ABCs (airway, breathing, circulation), which include providing oxygen, controlling severe hemorrhage, and initiating intravenous (IV) fluids to maintain hemodynamic stability; airway control may be necessary for a large intracranial hemorrhage.
- Emergency department care. Life-threatening bleeding requires conventional critical care interventions; in the patient with known ITP, high-dose parenteral glucocorticoids and IV immunoglobulin (IVIg), with or without platelet transfusions, are appropriate.
- Consultations. Consult a hematologist for assistance in confirming the diagnosis or, in the patient with known ITP, arranging disposition and follow-up care, if appropriate.
Pharmacologic Management
Glucocorticoids and intravenous immunoglobulin (IVIg) are the mainstays of medical therapy for idiopathic thrombocytopenic purpura (ITP).
- Glucocorticoids. These agents are used to treat idiopathic and acquired autoimmune disorders; they have been shown to increase platelet count in ITP.
- Blood products. Administration of IVIg may temporarily increase platelet counts in some children and adults with ITP; consider IVIg if the situation requires a rapid, temporary rise in platelet count.
- Thrombopoietic. These agents directly stimulate bone marrow platelet production.
Nursing Management
Nursing care for a child with idiopathic thrombocytopenia purpura include:
Nursing Assessment
Assessment of a child with ITP includes the following:
- History. Medications can be a common etiology for inducing thrombocytopenia, and patients should have their medications carefully reviewed; one study used three distinct methods to document drugs that may be associated with drug-induced immune thrombocytopenia (DITP).
- Physical exam. Address risk factors for increased bleeding, such as GI disease, CNS disease, urologic disease, or active lifestyle, as these may determine the aggressiveness of management.
Nursing Diagnoses
Based on the assessment data, the major nursing diagnoses for idiopathic thrombocytopenic purpura are:
- Risk for bleeding related to decreased platelet count.
- Risk for injury related to abnormal blood profile.
- Risk for ineffective protection related to altered kinesthetic perception.
- Risk for infection related to suppression of the immune system by steroids.
Nursing Care Planning and Goals
The major nursing care planning goals for idiopathic thrombocytopenic purpura are:
- Patient or caregivers take measures to prevent bleeding and recognize signs of bleeding that need to be reported immediately to a health care professional.
- Patient does not experience bleeding as evidenced by normal blood pressure, stable hematocrit and hemoglobin levels and desired ranges for coagulation profiles.
- Patient remains free of injuries.
- Patient increases daily activity, if feasible.
- Patient remains free of infection, as evidenced by normal vital signs and absence of signs and symptoms of infection.
- Early recognition of infection to allow for prompt treatment.
Nursing Interventions
Nursing interventions for a child with ITP are:
- Prevent bleeding. Review laboratory results for coagulation status as appropriate: platelet count, prothrombin time/international normalized ratio (PT/INR), activated partial thromboplastin time (aPTT), fibrinogen, bleeding time, fibrin degradation products, vitamin K, activated coagulation time (ACT); and educate the at-risk patient and caregivers about precautionary measures to prevent tissue trauma or disruption of the normal clotting mechanisms.
- Prevent injury. Thoroughly conform patient to surroundings; put call light within reach and teach how to call for assistance; respond to call light immediately; avoid use of restraints; obtain a physician’s order if restraints are needed; and eliminate or drop all possible hazards in the room such as razors, medications, and matches.
- Prevent infection. Wash hands and teach patient and SO to wash hands before contact with patients and between procedures with the patient; encourage fluid intake of 2,000 to 3,000 mL of water per day, unless contraindicated; recommend the use of soft-bristled toothbrushes and stool softeners to protect mucous membranes; and if infection occurs, teach the patient to take antibiotics as prescribed; instruct patient to take the full course of antibiotics even if symptoms improve or disappear.
Evaluation
Goals are met as evidenced by:
- Patient or caregivers took measures to prevent bleeding and recognized signs of bleeding that need to be reported immediately to a health care professional.
- Patient did not experience bleeding as evidenced by normal blood pressure, stable hematocrit and hemoglobin levels and desired ranges for coagulation profiles.
- Patient remained free of injuries.
- Patient increased daily activity, if feasible.
- Patient remained free of infection, as evidenced by normal vital signs and absence of signs and symptoms of infection.
- Early recognition of infection allowed for prompt treatment.
Documentation Guidelines
Documentation in a child with ITP include the following:
- Baseline and subsequent assessment findings to include signs and symptoms.
- Individual cultural or religious restrictions and personal preferences.
- Plan of care and persons involved.
- Teaching plan.
- Client’s responses to teachings, interventions, and actions performed.
- Attainment or progress toward the desired outcome.
- Long-term needs, and who is responsible for actions to be taken.




























Leave a Comment